International consortium investigates overactive immune cells as cause of COVID-19 deaths
New publication links neutrophil infiltration in the lungs of patients to COVID-19 symptoms
Montreal, April 16, 2020 – In the urgent battle to treat COVID-19 patients, a group of eleven international medical research organizations is investigating whether overactive immune cells that produce Neutrophil Extracellular Traps (NETs) cause the most severe cases. The consortium, called the NETwork, includes Cold Spring Harbor Laboratory, the Feinstein Institutes for Medical Research, and the Research Institute of the McGill University Health Centre (RI-MUHC).
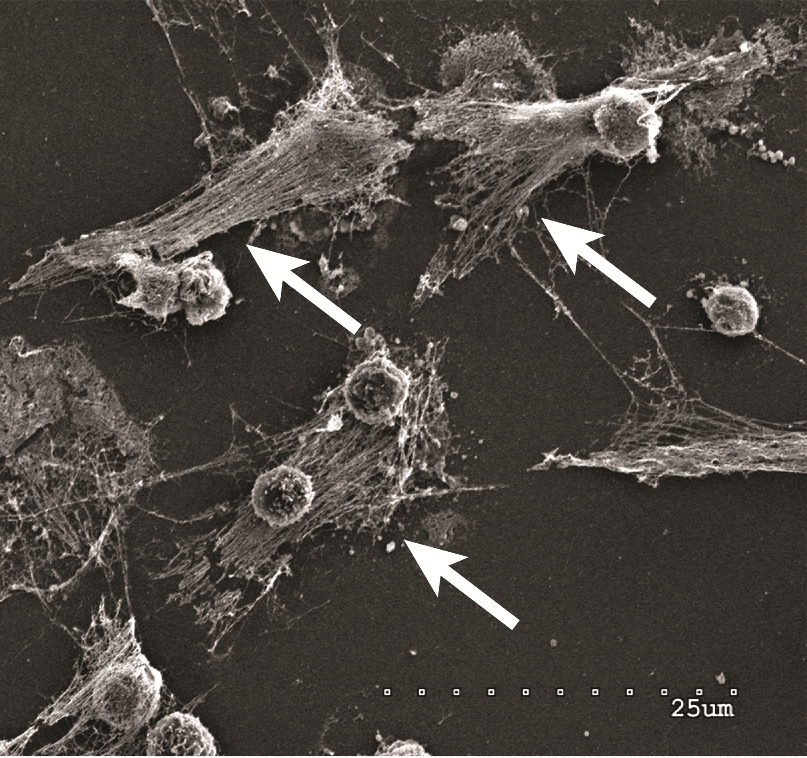
Figure 1. Part of the body’s immune system, neutrophils detect bacteria and can expel their DNA (see arrows) to attack the bacteria with a gauzy web of DNA laced with toxic enzymes, called a NET.
A paper published today in the Journal of Experimental Medicine describes that patients with severe COVID-19 infection develop Acute Respiratory Distress Syndrome (ARDS), pulmonary inflammation, thick mucus secretions in the airways, extensive lung damage, and blood clots. This late stage of the disease is difficult to manage. In the worst cases, patients require invasive mechanical ventilation, and still, a large number of patients die. The NETwork suggests that the severity of COVID-19 may result from overactive white blood cells known as the neutrophils. Part of the body’s immune system, neutrophils detect bacteria and can expel their DNA to attack the bacteria with a gauzy web of DNA laced with toxic enzymes, called a NET. These NETs can ensnare and digest the unwanted pathogen but in cases of ARDS, they damage the lungs and other organs.“Given the clear similarities between the clinical presentation of severe COVID-19 and other known diseases driven by NETs, such as ARDS, we propose that excess NETs may play a major role in the disease,” said Betsy Barnes, PhD, lead and co-corresponding author of the paper and professor at the Feinstein Institutes. “As samples from patients become available, it will be important to determine whether the presence of NETs associates with disease severity and/or particular clinical characteristics of COVID-19.”
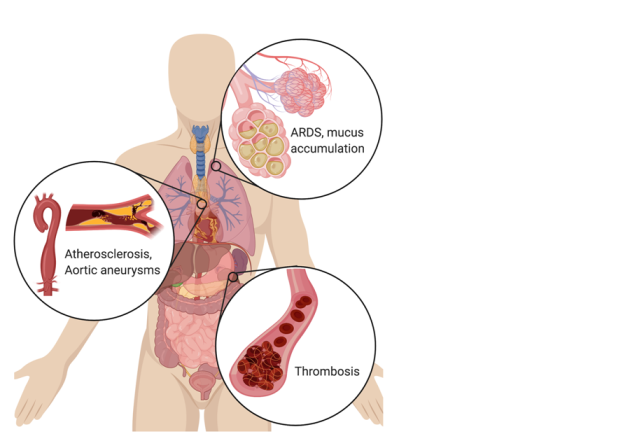
Figure 2. Excess NET formation can drive a variety of severe pathologies. In the lungs, NETs drive the accumulation of mucus in cystic fibrosis patients’ airways. NETs also drive acute respiratory distress syndrome (ARDS) after a variety of inducers, including influenza. In the vascular system, NETs drive atherosclerosis and aortic aneurysms, as well as thrombosis (particularly microthrombosis), with devastating effects on organ function.
“NETs were identified in 2004, but many scientists have never heard of them. Most of the researchers in the NETwork have worked on NETs in other diseases, and when we started hearing about the symptoms of the COVID-19 patients, it sounded familiar,” said Cold Spring Harbor Laboratory cancer biologist Mikala Egeblad, PhD, who coalesced the NETwork research group around COVID-19 and is senior and corresponding author of the paper.
Jonathan Spicer, MD PhD, a clinician scientist at the RI-MUHC and assistant professor of Surgery at McGill University is a thoracic surgeon who has witnessed the devastating effects of COVID-19 infection at the bedside. “We see in these patients severe lung damage known as ARDS, another serious problem caused by excess NETs and seen in cases of severe influenza,” he said. “In addition, their airways are often clogged with thick mucus and unlike most severe lung infections, these patients tend to form small clots throughout their body at much higher rates than normal. NETs have also been found in the blood of patients with sepsis or cancer, where they can facilitate the formation of such blood clots.”

Researchers at the eleven NETwork institutions are now pursuing studies into whether NETs are a common feature in COVID-19 cases. If their findings show that excess NETs cause the severe symptoms of COVID-19, then a new avenue of treatments may be deployed to help COVID-19 patients. Current treatments used in other NET and neutrophil-driven diseases–like cystic fibrosis, gout, and rheumatoid arthritis–might dampen the activity of NETs in COVID-19 patients, reducing the need for invasive mechanical ventilation.
The following research institutes comprise the NETwork: Cold Spring Harbor Laboratory, The Feinstein Institutes for Medical Research, McGill University Health Centre, Weill Cornell Medicine, Donald and Barbara Zucker School of Medicine at Hofstra/Northwell, Centre Hospitalier Universitaire de Nancy, University of Michigan, University of California, San Francisco, University of Texas MD Anderson Cancer Center, University of Utah School of Medicine, and Northwell Health.
Video: How NETs harm lungs (Source CSHL)
About Cold Spring Harbor Laboratory
Founded in 1890, Cold Spring Harbor Laboratory has shaped contemporary biomedical research and education with programs in cancer, neuroscience, plant biology and quantitative biology. Home to eight Nobel Prize winners, the private, not-for-profit Laboratory is a National Cancer Institute designated Cancer Center, employing 1,100 people including 600 scientists, students and technicians. The Meetings & Courses Program annually hosts more than 12,000 scientists. The Laboratory’s education arm also includes an academic publishing house, a graduate school and the DNA Learning Center with programs for middle and high school students and teachers. For more information, visit www.cshl.edu
About the Feinstein Institutes
The Feinstein Institutes for Medical Research is the research arm of Northwell Health, the largest health care provider and private employer in New York State. Home to 50 research labs, 2,500 clinical research studies and 5,000 researchers and staff, the Feinstein Institutes raises the standard of medical innovation through its five institutes of behavioral science, bioelectronic medicine, cancer, health innovations and outcomes, and molecular medicine. We make breakthroughs in genetics, oncology, brain research, mental health, autoimmunity, and are the global scientific leader in bioelectronic medicine – a new field of science that has the potential to revolutionize medicine. For more information about how we produce knowledge to cure disease, visit feinstein.northwell.edu.
About the Research Institute of the McGill University Health Centre
The Research Institute of the McGill University Health Centre (RI-MUHC) is a world-renowned biomedical and healthcare research centre. The Institute, which is affiliated with the Faculty of Medicine of McGill University, is the research arm of the McGill University Health Centre (MUHC) – an academic health centre located in Montreal, Canada, that has a mandate to focus on complex care within its community. The RI-MUHC supports over 460 researchers and close to 1,300 research trainees devoted to a broad spectrum of fundamental, clinical and health outcomes research at the Glen and the Montreal General Hospital sites of the MUHC. Its research facilities offer a dynamic multidisciplinary environment that fosters collaboration and leverages discovery aimed at improving the health of individual patients across their lifespan. The RI-MUHC is supported in part by the Fonds de recherché du Québec – Santé (FRQS). rimuhc.ca
CSHL Contact:
Dagnia Zeidlickis
516-367-6846
[email protected]
Feinstein Contact:
Matthew Libassi
516-465-832
[email protected]
RI-MUHC Contact:
Fabienne Landry
514-812-7722
[email protected]