First-of-their-kind wearables capture body sounds to continuously monitor health
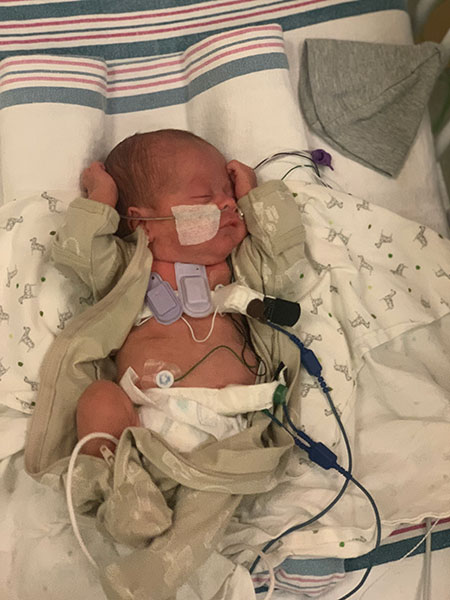
The Montreal Children’s Hospital participated in a study that tested new devices on a range of patients, including premature babies.
Montreal, November 16, 2023 - During even the most routine visits, physicians listen to sounds inside their patients’ bodies — air moving in and out of the lungs, heart beats and even digested food progressing through the long gastrointestinal tract. These sounds provide valuable information about a person’s health. And when these sounds subtly change or downright stop, it can signal a serious problem that warrants time-sensitive intervention.
As announced by Northwestern University in a press release today, researchers are introducing new soft, miniaturized wearable devices that go well beyond episodic measurements obtained during occasional doctor exams in a new study just published in the journal Nature Medicine. Softly adhered to the skin, the devices continuously track these subtle sounds simultaneously and wirelessly at multiple locations across nearly any region of the body.
In pilot studies, researchers tested the devices on 15 premature babies with respiratory and intestinal motility disorders and 55 adults, including 20 with chronic lung diseases. Not only did the devices perform with clinical-grade accuracy, they also offered new functionalities that have not been developed nor introduced into research or clinical care.
“Currently, there are no existing methods for continuously monitoring and spatially mapping body sounds at home or in hospital settings,” said Northwestern’s John A. Rogers, a bioelectronics pioneer who led the device development. “Physicians have to put a conventional, or a digital, stethoscope on different parts of the chest and back to listen to the lungs in a point-by-point fashion. In close collaborations with our clinical teams, we set out to develop a new strategy for monitoring patients in real-time on a continuous basis and without encumbrances associated with rigid, wired, bulky technology.”
Non-obtrusively monitoring babies’ breathing
When developing the new devices, the researchers had two vulnerable communities in mind: premature babies in the neonatal intensive care unit (NICU) and post-surgery adults.
Particularly common in premature babies, apneas are a leading cause of prolonged hospitalization and potentially death. When apneas occur, infants either do not take a breath (due to immature breathing centers in the brain) or have an obstruction in their airway that restricts airflow. Some babies might even have a combination of the two. Yet, there are no current methods to continuously monitor airflow at the bedside and to accurately distinguish apnea subtypes, especially in these most vulnerable infants in the clinical NICU.
In collaborative studies conducted at the Montreal Children’s Hospital, healthcare workers placed the acoustic devices on babies just below the suprasternal notch at the base of the throat. Devices successfully detected the presence of airflow and chest movements and could estimate the degree of airflow obstruction with high reliability, therefore allowing identification and classification of all apnea subtypes.
“When placed on the suprasternal notch, the enhanced ability to detect and classify apneas could lead to more targeted and personalized care, improved outcomes and reduced length of hospitalization and costs,” said Dr. WissamShalish, a neonatologist at the Montreal Children’s Hospital, junior scientist in the Child Health and Human Development Program at the Research Institute of the McGill University Health Centre, and co-first author of the study.
“When placed on the right and left chest of critically ill babies, the real-time feedback transmitted whenever the air entry is diminished on one side relative to the other could promptly alert clinicians of a possible pathology necessitating immediate intervention.”
Tracking infant digestion
In children and infants, cardiorespiratory and gastrointestinal problems are major causes of death during the first five years of life. Gastrointestinal issues, in particular, are accompanied by reduced bowels sounds, which could be used as an early warning sign of digestion issues, intestinal dysmotility and potential obstructions. So, as part of the pilot study in the NICU, the researchers used the devices to monitor these sounds.
In the study, premature babies wore sensors at four locations across their abdomen. Early results aligned with measurements of adult intestinal motility using wire-based systems, which is the current standard of care.
“When placed on the abdomen, the automatic detection of reduced bowel sounds could alert the clinician of an impending (sometimes life-threatening) gastrointestinal complication,” Shalish said. “While improved bowel sounds could indicate signs of bowel recovery, especially after a gastrointestinal surgery.”
In addition to offering continuous monitoring, the devices also untethered NICU babies from the variety of sensors, wires and cables connected to bedside monitors.
To learn more, read the Northwestern University press release.
About the study
The study Wireless broadband acousto-mechanical sensors as body area networks for continuous physiological monitoring was conducted by Jae-Young Yoo, Seyong Oh, WissamShalish, Woo-YoulMaeng, Emily Cerier, Emily Jeanne, Myungkun Chung, ShashaLv, Yunyun Wu, SeonggwangYoo, Andreas Tzavelis, Jacob Trueb, Minsu Park, HyoyoungJeong, EfeOkunzuwa, SlobodankaSmilkova, Gyeongwu Kim, Junha Kimi Gooyoon Chung, Yoonseok Park, Anthony Banks, Shuai Xu, Guilherme M. Sant’Anna, Debra E. Weese-Mayer, Ankit Bharat and John A. Rogers.
https://doi.org/10.1038/s41591-023-02637-5
