Portrait of a telehealth visionary
A leader with a passionate disposition and devotion to her work, Madeleine St-Gelais has spent more than 12 years developing telehealth within the Réseau universitaire intégré de santé McGill (RUIS McGill). Her outstanding contribution to the service in Quebec earned Madeleine St-Gelais the 2006 Alain Cloutier Award of Excellence. A nurse with a master’s degree in public administration, she is concerned about the health and welfare of deprived communities in isolated regions of Quebec. Her sensitivity to their situation is matched only by the energy she has invested in providing them with better access to care.
We met with Madeleine in December, just before her retirement.

How did you become part of the McGill Telehealth team?
In 2003, I met Johanne Desrochers [who was, until recently, the RUIS McGill Telehealth Co-Chair] at a conference about telehealth. She had a number of questions about access to care that I had been thinking about myself for several years because I was working in a remote area in Quebec Lower North Shore. A short time later, she invited me to help her develop telehealth at the McGill University Health Centre (MUHC), and I accepted. That’s how the adventure began.
But what is telehealth exactly? What is it used for?
Telehealth is about providing health services at a distance, such as care, training, research or clinical management. But we’re developing the clinical aspect as a priority. We offer diagnostic, follow-up, and treatment services to the regions so patients have access to care that meets their needs closer to home.
Can you give a few examples?
We’ve created a virtual health and social services centre (CvSSS), which now provides integrated clinical services in more than 35 specialties, with more than 1,000 participants (physicians and others).
Teleconsultations take place every day in several specialties in a number of Quebec regions. We’ve set up a platform to receive and prioritize teleconsultation requests, to carry out exchanges between professionals or with patients, in real or delayed time, and to send reports to referring physicians. All of this is done electronically, confidentially and securely. Doctors can even handle equipment remotely. It’s like having virtual clinics with doctors who are available on demand by videoconference.
An example is screening for diabetic retinopathy among the Cree, a condition that can lead to blindness if left untreated. Images of the retina are taken locally by trained personnel and then transmitted electronically to specialists for interpretation and diagnosis. If there is retinopathy, the patient then has access to appropriate follow-up. Today, we’re proud to say that we have done about 3,000 screenings, avoided as many trips to Montreal, saved millions of dollars and, above all, saved eyes.
There are so many other projects worth mentioning, such as the school-to-hospital project, through which children in hospital can continue their education; telehomecare, which permits patients with chronic illnesses to receive personalized follow-up at home; and, of course, the telethrombolysis project, which allows for the evaluation and treatment of stroke victims 24 hours per day, seven days a week.
What area do you cover?
We serve the RUIS McGill territory, which covers 63 per cent of the area of Quebec. In addition, thanks to the expertise developed by our team and the strength of our infrastructure, we provide technological support outside this area, notably for the territory of the RUIS de l’Université de Montréal for telehealth activities and for West-Central and Western Quebec for telethrombolysis.
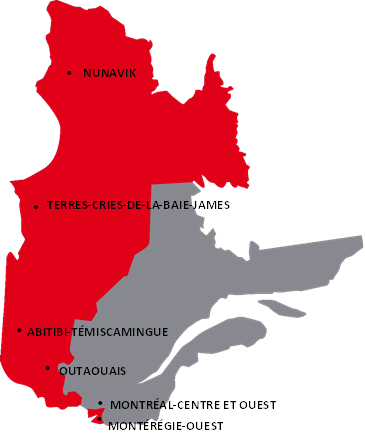
Source : RUIS McGill
What project are you most proud of?
I would say that the best gift we’ve given to the regions is the pooling of shareable clinical applications. In simple terms, we’ve made certain that MUHC clinical applications are available to other institutions. For example, if a patient has an electrocardiogram (ECG) in Nunavik, the result is saved in the MUHC application database, interpreted by a physician, and the report is sent to the referring physician. It works the same way for other tests, such as the fetal activity test, which allows pregnant women to be monitored remotely.
How were you able to coordinate and accomplish all these projects?
It was the work of a team whose vision is to connect first-to third-line partners to improve accessibility and continuity of services. Together, we’ve created an infrastructure capable of supporting a continually growing number of services.
We’ve established a single point of access, which connects providers to those needing care and offers training and technical support as well as support for the development of new services and the management of telehealth projects.
You’re about to pass the torch. What challenges are your colleagues facing?
They’ll need to develop new partnerships, sensitize the clinical community to the needs of people in isolated areas and work to change regulations that sometimes limit the development of telehealth. Of course, they’ll have to keep up with technological changes, as we have done, from the workstation, the cell phone, to the tablet.
My dream is that telehealth will become well integrated into practice and that any professional will be able to work seamlessly in a virtual or traditional manner.
I’m optimistic because the young doctors were born with electronics. It’s going to become increasingly simple.
What is telehealth?
The Act Respecting Health and Social Services defines telehealth as “a health or social services-related activity, service or system that is practised, provided or delivered in Québec from a distance for educational, diagnostic or treatment purposes or for purposes of research, clinical management or training, using information and communications technologies.” Telehealth services do not include telephone consultations. The legislation defines telehealth as a way of delivering services applicable to all traditional fields of practice.
Telehealth allows for the remote use of biomedical equipment, ranging from the electronic stethoscope to the most complex medical imaging equipment for diagnostic purposes, and the development of treatment plans.
Telemonitoring applications, such as telehomecare, not only allow healthcare professionals to remotely monitor patients’ clinical data but also to contribute to their autonomy by helping them understand and manage their health.
These examples are just illustrations of how telehealth can be used to facilitate and improve service delivery for patients and caregivers.
Increasing volumes in 2015-2016
Videoconference
- 53,780 videoconferencing sessions throughout RUIS McGill, an increase of 70% over the previous year.
- 19 % of the sessions were related to clinical activities and 39 % were related to training.
Teleconsultations
- 10,959 direct, indirect and time-delayed teleconsultations, double the amount of the preceding year.