Healthcare at Your Fingertips
Digital Health Week (from November 12-18) is an annual celebration and recognition of how digital health is transforming the delivery of care across the country. With this year’s themes of ‘Faster, More Efficient Care’, ‘Virtual Visits’ and ‘Accessing your Lab Results and Personal Information’, we are proud to showcase some apps being developed by teams at the McGill University Health Centre (MUHC).
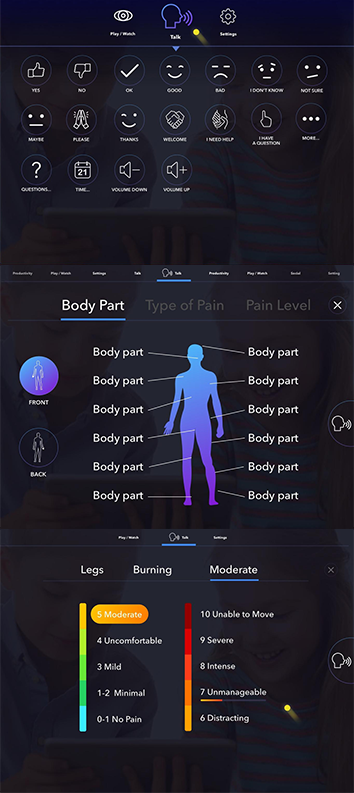 | PigioLaunch Date: Early 2019. What is it? Pigio is a communication tool for patients unable to speak due to paralysis resulting from a stroke, ALS or temporary loss of speech. Patients control a cursor on a computer screen using only their eye movements thanks to eye-tracking technology and the embedded camera of the smart device. This allows for rapid communication with others since the patient can select pre-defined sentences and words displayed on the screen. Who is behind it? Dr. Étienne de Villers-Sidani, cognitive neuroscientist at the Montreal Neurological Institute and Hospital. What does it do? “Piggio requires no third party equipment and is only a fraction of the price of current eye-tracking technologies,” says Dr. De Villers-Sidani. “By making this technology affordable, we aim to improve the standard of care by helping healthcare professionals communicate with patients in a hospital setting, as well as improving the ability of patients to communicate with their loved ones in their day-to-day lives.” Who funded it? Pre-seed angel funding. |
| AideSmart!Launch Date: Currently in use in a pilot project; coming soon. What is it? AideSmart! is a novel infection screening and counselling app that simultaneously provides point-of-care tests and a counselling service. It engages participants by linking them to care for timely screening and treatment of HIV and STIs, including Hepatitis B and C viruses, and syphilis. Who is behind it? Dr. Nitika Pant Pai, researcher at the Research Institute, and Associate Professor in McGill University’s Department of Medicine. What does it do? "AideSmart! offers healthcare professionals rapid testing services inside the clinic, including screening, pre-and-post-test combined counselling and referral, confirmatory testing, and links to getting further care,” says Dr. Pai. “It not only communicates with patients but expands the reach and functionality of point-of-care tests by connecting laboratory technicians, labs, physicians and professionals involved in service delivery.” Who funded it? Grand Challenges Canada and Canadian Institutes of Health Research. |
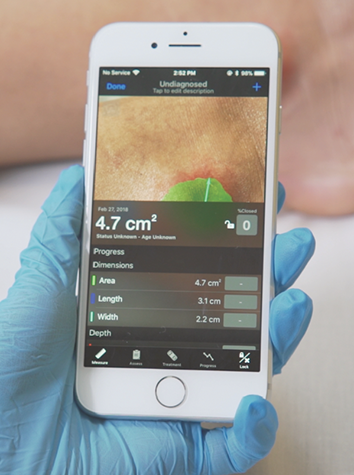 | Swift Skin and WoundLaunch Date: Currently in use in over 1,000 healthcare facilities. What is it? Swift Skin and Wound is a smartphone app used to photograph, measure, and document wounds, and makes this information available for remote clinicians and administrators. These wound measurements are more reliable and accurate than those taken through the use of a ruler as is the current standard of care. Who is behind it? Co-founded by Dr. Sheila Wang, resident in Dermatology in the Department of Medicine at McGill University and scientist at the Research Institute of the MUHC. What does it do? “The app’s ability to reliably and accurately measure wound area, even by those with limited experience, means that it is well-positioned to have a significant impact on clinical management plus patient outcomes. Swift’s enterprise-grade solution streamlines clinical and administrative wound care management workflows, from image capture and automatic risk scoring, to assessment scheduling and claims submission.” Who funded it? Swift Medical. |
 | The CDH (Congenital Diaphragmatic Hernia) Clinical Guideline AppLaunch Date: October 2018. What is it? CDH is a "hole" in the diaphragm muscle through which the intestines can move into the chest. This app provides rapid access to recommendations for all phases of CDH care from prenatal diagnosis to hospital discharge and follow-up; links to calculators for key patient data; a daily ICU rounding checklist and flowsheet; a guideline compliance checklist for quality improvement; and access to full guidelines with expanded discussions and complete references. Who is behind it: Dr. Pramod Puligandla, pediatric surgeon and intensivist, Department of Pediatric Surgery, Montreal Children’s Hospital (MCH); and Dr. Kathryn LaRusso, research fellow, Department of Pediatric Surgery, Montreal Children’s Hospital (MCH). What does it do? “The goal of the app is to improve outcomes for children with congenital diaphragmatic hernia," says Dr. Puligandla. “The app provides easy access to tools and resources useful to all clinicians involved in the care of children with CDH." Who funded it? Medical Staff Services Association Innovation Grant at the MCH and from Stradigi AI Inc. |
