Which artificial pancreas system is the best for children with type 1 diabetes?
A Montréal research team, co-supervised by Dr. Rémi Rabasa-Lhoret from the IRCM and Dr. Laurent Legault from the Montreal Children’s Hospital (MCH) and the Research Institute of the McGill University Health Centre (RI-MUHC), undertook the first paediatric outpatient study to compare three alternative treatments for type 1 diabetes. The results, published this week in the scientific journal The Lancet Diabetes & Endocrinology, shows the dual-hormone artificial pancreas provides the most benefits by reducing the time spent in nocturnal hypoglycaemia.
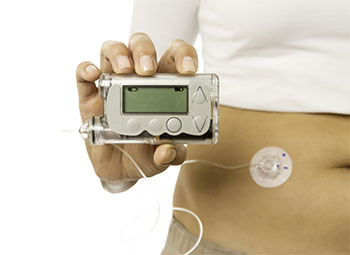 The study conducted with children and adolescents with type 1 diabetes aimed to measure the effectiveness of three strategies in reducing nocturnal hypoglycemia. Taking place over multiple nights at a diabetes camp last summer, the trial compared conventional insulin pump therapy with two configurations of the external artificial pancreas being developed at the IRCM: the single-hormone (insulin alone) artificial pancreas and the dual-hormone (insulin and glucagon) artificial pancreas.
The study conducted with children and adolescents with type 1 diabetes aimed to measure the effectiveness of three strategies in reducing nocturnal hypoglycemia. Taking place over multiple nights at a diabetes camp last summer, the trial compared conventional insulin pump therapy with two configurations of the external artificial pancreas being developed at the IRCM: the single-hormone (insulin alone) artificial pancreas and the dual-hormone (insulin and glucagon) artificial pancreas.
“The dual-hormone artificial pancreas has the potential to reduce hypoglycemia more than the other strategies, but the relative benefits provided by glucagon had not yet been assessed in outpatient settings,” says Dr. Rabasa-Lhoret, endocrinologist and clinical researcher at the IRCM. “Demonstrating the effectiveness of the artificial pancreas among children in an uncontrolled environment is an important step in making this technology available to the general public in the near future.”
Patients with type 1 diabetes must maintain their blood glucose levels within a target range in order to prevent serious long-term complications related to high glucose levels and reduce the risk of hypoglycemia (very low blood glucose that can lead to confusion, disorientation and, if severe, loss of consciousness, coma and seizure). Results from the study showed the dual-hormone artificial pancreas increased the percentage of time spent within this recommended target range.
“During our study, we also found that no participant using the dual-hormone system experienced a nocturnal hypoglycaemia event requiring treatment,” explains Ahmad Haidar, PhD, engineer and postdoctoral fellow at the IRCM. “This is significant when considering that hypoglycaemic events occurred on 16 per cent of nights with conventional pump therapy, and 4 per cent of nights with the single-hormone artificial pancreas.”
“Most hypoglycaemia seizures in children and adolescents happen at night-time, and fear of these episodes is a major source of stress and anxiety for families and caregivers of children with type 1 diabetes,” mentions Dr. Legault, paediatric endocrinologist at the MCH and a researcher in Endocrinology and Metabolism at the RI-MUHC. “This represents a major barrier to efforts to intensify treatment in order to reach glycemic targets.”
“The dual-hormone artificial pancreas could improve nocturnal glucose control and reduce hypoglycaemia, potentially improving quality of life, but it also requires an extra catheter and additional drug manipulation,” adds Dr. Rabasa-Lhoret. “Longer and larger outpatient studies are now needed to assess whether it is justifiable to add glucagon to the artificial pancreas. To predict future adherence to dual-hormone therapy, we also need to assess, from patients’ perspectives, whether the clinical benefits outweigh the increased cost and complexity.”
Type 1 diabetes is one of the most common chronic diseases in young people and, each year, its incidence is increasing by two to five per cent worldwide. According to the Canadian Diabetes Association, more than 10 million Canadians are living with diabetes or prediabetes today. About five to 10 per cent of them have type 1 diabetes.
The research project was funded by the Canadian Diabetes Association, Dr. Rabasa-Lhoret’s J.A. De Sève Chair in clinical research, and Dr. Haidar’s Banting postdoctoral fellowship. The study’s authors include Laurence Matteau-Pelletier, Virginie Messier and Maryse Dallaire from the IRCM, as well as Martin Ladouceur from CRCHUM (research centre from the Centre hospitalier de l’Université de Montréal).